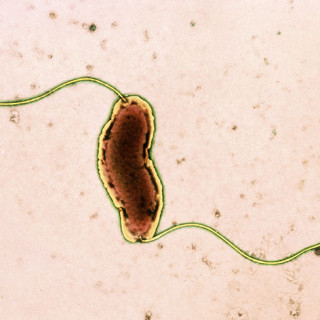
Breast milk protein can become a new weapon against resistant bacteria
Research is already underway on how the breast milk protein HAMLET can be used to treat cancer. Findings from Lund University indicate that it may even kill two types of respiratory bacteria. At the same time, the protein can make partially resistant bacteria – which every year claim many lives – to once again become susceptible to antibiotics.
NOW THE ROLE OF BREAST MILK PROTEIN in respiratory infections is to be studied more closely, and the person responsible for the project is Anders Håkansson, professor at the Institute for Translational Medicine:
“HAMLET can make resistant bacteria to once again become susceptible to antibiotics. This is one of the first substances where this ability is deemed secure”, he says.
The focus is now on a new combination treatment that neutralises the two respiratory bacteria Mycobacterum tuberculosis and Streptococcus pneumoniae. Each year, between three and four million people die from tuberculosis, pneumonia, sepsis or other bacterial diseases. There are now strains of Mycobacterum tuberculosis that are completely resistant to all antibiotics used in conventional practice. Also Streptococcus pneumoniae are highly resistant to several different antibiotics around the world.
“A compound from breast milk can make bacteria react to ineffective antibiotics”.
HAMLET (Human Alpha-lactalbumin Made Lethal to Tumour cells) is a compound of proteins and lipids (fats and fat-like substances) from breast milk. Previous research trials have already shown the protective effects it has on various cancers, but what’s new is that HAMLET has also proven to be an effective weapon against the two airborne bacteria. This generates a process in the bacteria similar to natural cell death.
Using the same mechanism that HAMLET employs to initiate cell death, it can also make the bacteria react to the weakened or ineffective antibiotics so that they once again become effective.
“HAMLET is also promising in terms of its ability to kill tuberculosis bacteria hiding in macrophages – a type of white blood cell which is part of the immune system. There the bacteria can be dormant and several years later cause new infections”, says Anders Håkansson.
THE RESEARCH IS CONDUCTED in collaboration with Dr. Michael Niederwies at the University of Alabama in Birmingham, USA, who is primarily knowledgeable within tuberculosis.
“We focus on two questions: How does HAMLET work, and how do we use it in treatment? We are identifying the molecules that are active when HAMLET causes bacterial death, and when the resistant bacteria become sensitive to antibiotics. Subsequently, we will test the effectiveness of a combination treatment. We will then use HAMLET and antibiotics in infection studies on mice”, explains Anders Håkansson and continues:
“Today a lot of antibiotics are prescribed around the world in the hope that they’ll work on respiratory bacteria. If we succeed with our research, a positive side effect would be that the use of antibiotics could decrease, and that the resistant bacterial strains become fewer. We will then break a vicious spiral.”
Text: Björn Martinsson
Published: 2015
Photo: Kennet Ruona